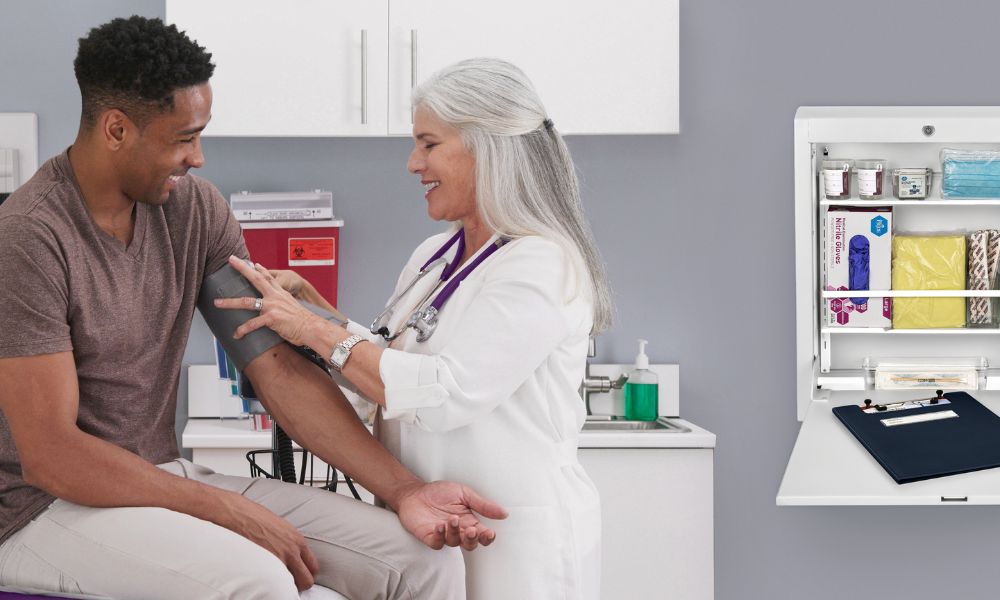
Accurate and comprehensive medical charting is a critical aspect of health care practice. Whether you’re a physician, nurse, or another type of health care professional, using proper charting ensures efficient communication, continuity of care, and legal documentation. However, navigating the intricacies of charting can be challenging. Below, we’ll explore the dos and don’ts of charting to help health care professionals maintain the highest standards of documentation.
Why Is Proper Charting Important?
Medical charts document a patient’s medical history. This information is extremely valuable to health care professionals such as yourself. For one, it provides you with a comprehensive overview of the patient’s past and current health conditions, medications, and treatments, aiding in accurate diagnosis and treatment planning.
Additionally, proper medical charting ensures effective communication among health care teams and promotes continuity of care. It also serves as a legal record, safeguarding both the patient and the health care provider in case of any medical or legal disputes.
The Dos of Charting
Properly charting your patients’ medical information is essential. Here are a few best practices you should follow to ensure the information you include in your patients’ charts is easy to read and accurate.
Document Promptly and Accurately
Make it a habit to document all patient encounters promptly and accurately. Timely documentation improves patient care and reduces the risk of errors. Include relevant information such as vital signs, symptoms, administered medications, and the patient’s response to treatment.
Use Clear and Concise Language
To convey information accurately, you’ll want to use clear and concise language in your documentation. Use standardized medical terminology, avoiding jargon or abbreviations. Remember that other health care professionals may need to interpret your notes, so aim for clarity and simplicity.
Write Slowly and Clearly
If you’re charting by hand, do so slowly and carefully. When you rush, you risk your handwriting becoming sloppy and illegible, which can cause future issues for both you and other health care professionals involved in the patient’s care. Your penmanship doesn’t need to be flawless, but you should ensure its readability.
Be Objective
Your charting should be objective and based on observed facts; avoid assumptions or speculation. Stick to the evidence and describe what you see, hear, and measure. For example, instead of writing, "The patient appears anxious," write, "The patient is fidgeting, has rapid breathing, and reports feeling restless."
Include Relevant Details
Make sure to include all relevant information in your charting. This includes main complaints, patient history, medications, allergies, test results, and any changes in the patient’s condition. Be thorough, but prioritize the information that’s most pertinent to the client’s current situation.
Use Dividers To Organize Information
Using dividers can help you organize your patients’ medical records. Dividers serve as visual markers that separate different sections within a patient’s chart, making it easier to quickly locate specific information.
By dividing the chart into sections—such as medical history, progress notes, test results, and treatment plans—health care professionals can navigate the chart and find information without wasting time.
Document Informed Consent
Whenever you perform a procedure or treatment, ensure the patient or their authorized representative provides informed consent. Document this consent in the patient’s chart. Also, be sure to include details of the discussion you had with the patient or their representative regarding risks, benefits, and alternative treatment options.
Collaborate With Other Health Care Professionals
Health care is a collaborative effort, and charting should reflect this. Coordinate with other health care professionals involved in the patient’s care to ensure you share all relevant information with each other. This includes consult notes and referrals.
The Don’ts of Charting
To prevent inaccurate, unhelpful, or biased information in your charting, you should avoid doing a few things.
Don’t Chart at the Beginning of an Appointment
Avoid charting at the beginning of a patient’s appointment. Instead, wait until you’ve finished providing care. A patient will provide you with foundational information about their symptoms, medical history, or current condition upon their arrival. However, as the appointment goes on, new information may come to light, and the patient’s condition may change or worsen. If you immediately chart the initial information without allowing for further observation and assessment, you risk capturing an incomplete or inaccurate picture of the patient’s health.
Don’t Alter or Backdate Records
Honesty and integrity are paramount when it comes to charting. Never alter or backdate records—this compromises the accuracy and legality of the documentation. If an error occurs, follow established protocols for making corrections, such as using a single-line strikeout with initials and a timestamp.
Avoid Subjective Language
Subjective language can be misleading and open to interpretation. Instead of using terms such as "normal" or "abnormal," provide objective measurements and comparisons. For example, instead of writing, "The patient’s wound looks better," document the wound’s size, color, and any signs of improvement or deterioration.
Don’t Assume Previous Entries Are Accurate
When reviewing a patient’s chart, don’t assume that previous entries are accurate or up to date. Verify information independently and make corrections if necessary. If there are discrepancies, communicate with the health care provider who made the original entry to ensure clarity and accuracy.
Avoid Copying and Pasting
While electronic health records (EHRs) have made charting more efficient, copying and pasting information from one note to another can result in inaccuracies. Each entry should reflect the patient’s current condition and individualize the care provided. If you do need to copy and paste, do so thoughtfully, ensuring the information remains relevant and applicable.
Don’t Forget To Sign and Date Entries
You need to sign and date every entry in a patient’s chart. This ensures accountability and allows other health care professionals to identify the correct timeline of events and actions taken regarding the patient’s care.
Now that you’re aware of the dos and don’ts of charting for health care professionals, you can ensure your patients’ records remain up-to-date and error-free. While charting can be frustrating and time-consuming, it’s one of the most important tasks you’ll perform on a day-to-day basis. By taking the time to fill out your patients’ medical charts with detailed and accurate information, you help them get the medical attention they need to remain happy and healthy.
At Carstens, we understand that properly charting medical information can be difficult, especially when you feel rushed during a busy shift. That’s why we offer a variety of supplies to make this crucial task easier. Using our chart dividers for medical records, you can keep your patients’ charts organized, allowing you to locate or jot down information quickly and efficiently. Browse our high-quality, USA-made supplies for medical professionals today.